Overuse Injuries in Athletes: Causes, Symptoms and Prevention
Overuse injuries are among the most frustrating conditions an active person can face. Unlike acute injuries — a sudden fracture, a ligament rupture, a dislocation — overuse injuries develop insidiously. There is no single moment of impact to point to, no obvious event to explain the pain. Instead, there is a gradual accumulation of stress on a tendon, joint, or bone that eventually exceeds the tissue’s capacity to repair itself. By the time the athlete seeks medical attention, the injury is often well established.
This pattern is particularly common in sports that involve repetitive upper limb loading — tennis, padel, golf, swimming, CrossFit, and throwing sports among them. The shoulder, elbow, and wrist bear the brunt of these demands, and when the balance between load and recovery is disrupted, injury follows. Understanding how overuse injuries develop, how they are diagnosed, and how they can be prevented is essential for any athlete who wants to train consistently and compete without interruption.
What is an Overuse Injury?
An overuse injury, also referred to as a repetitive strain injury (RSI), occurs when cumulative mechanical stress on a tissue exceeds its capacity to adapt and recover. This happens when training load increases too rapidly, recovery is insufficient, or biomechanical inefficiencies place abnormal stress on specific structures.
Unlike acute injuries, there is no discrete moment of tissue failure. Instead, micro-damage accumulates faster than the body can repair it. Over time, this leads to structural changes — tendon degeneration, stress reactions in bone, or chronic joint inflammation — that manifest as pain, weakness, and functional limitation.
In athletes, the tissues most commonly affected are:
- Tendons — the most frequent site of overuse pathology
- Bursae — fluid-filled sacs that can become chronically inflamed under repetitive stress
- Bone — subject to stress reactions and stress fractures with high-volume loading
- Cartilage — particularly in joints subjected to repetitive compressive or shearing forces
The upper limb is disproportionately affected in many sports, and the elbow, shoulder, and wrist are the joints most frequently seen in a sports injury clinic.
Common Upper Limb Overuse Injuries in Athletes
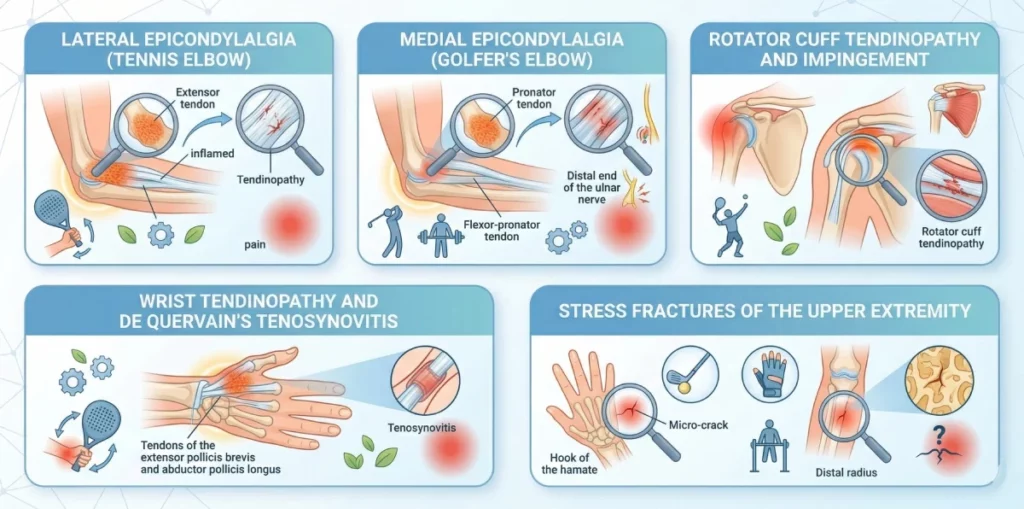
Lateral Epicondylalgia (Tennis Elbow)
Despite its name, tennis elbow affects far more non-tennis players than tennis players. It is the most common overuse injury of the elbow, caused by repetitive loading of the extensor tendons at their attachment on the lateral epicondyle.
In recent years, padel has become one of the most significant contributors to this condition in the UAE and across the region. The sport’s high-frequency wrist and forearm movements — particularly the smash and the bandeja — place repetitive eccentric demands on the extensor tendons that, without adequate recovery, lead to tendinopathy.
Symptoms include pain on the outer aspect of the elbow, weakness of grip, and discomfort during activities involving wrist extension or forearm rotation.
Medial Epicondylalgia (Golfer’s Elbow)
The medial equivalent of tennis elbow, this condition involves the flexor-pronator tendon origin at the medial epicondyle. It is seen in golfers, throwers, and increasingly in CrossFit athletes who perform high volumes of pulling movements.
Symptoms include pain on the inner elbow, often with associated tingling in the ring and little fingers if the adjacent ulnar nerve is irritated.
Rotator Cuff Tendinopathy and Impingement
The rotator cuff — a group of four muscles and their tendons that stabilise and move the shoulder — is highly vulnerable to overuse in overhead athletes. Swimmers, tennis players, padel players, and throwing athletes are particularly at risk.
Repetitive overhead motion, combined with any deficiency in scapular control or rotator cuff strength, creates a pattern of subacromial impingement — where the tendons are repeatedly compressed between the humeral head and the acromion. Over time, this leads to tendinopathy, bursitis, and — in some cases — partial or full-thickness tears.
Wrist Tendinopathy and De Quervain’s Tenosynovitis
The wrist tendons are subject to significant repetitive loading in racket sports and climbing. De Quervain’s tenosynovitis — inflammation of the tendons on the thumb side of the wrist — is particularly common in padel players and golfers.
Symptoms include pain and swelling on the radial aspect of the wrist, aggravated by gripping and thumb movement.
Stress Fractures of the Upper Extremity
While less common than in the lower limb, stress fractures can occur in the upper extremity — particularly in the hook of the hamate (common in golfers and batting sports) and the distal radius (in gymnasts and weightlifters). These require prompt diagnosis to prevent progression to complete fracture.
How Overuse Injuries Are Diagnosed
Accurate diagnosis is essential — not just confirming that an overuse injury is present, but understanding the specific structure involved, the severity of the pathology, and the contributing factors. A surface-level diagnosis leads to surface-level treatment.
A thorough assessment by an experienced sports injury doctor involves:
Clinical history — understanding the sport, training volume and recent changes, symptom onset and progression, and previous injuries or treatments.
Physical examination — palpation, provocative tests, and assessment of strength, range of motion, and biomechanics. In elbow tendinopathy, for instance, specific provocation tests can distinguish lateral from medial pathology and identify any nerve involvement.
Imaging — plain X-rays are useful for identifying bony pathology, calcification, or joint changes. Ultrasound is particularly valuable for dynamic assessment of tendons and bursae. MRI provides the most detailed soft tissue characterisation and is used when tendon tears, stress fractures, or intra-articular pathology are suspected.
The combination of clinical assessment and targeted imaging allows for a precise diagnosis that guides treatment decisions.
Treatment Principles for Overuse Injuries
The approach to overuse injuries has evolved considerably over the past decade. The old model of rest-and-wait has given way to a more active, structured approach.
Load Management
The first and most important intervention is load modification — not necessarily complete rest, but a reduction in the volume and intensity of the aggravating activity to a level the tissue can tolerate. This creates the conditions for healing without the deconditioning that comes with prolonged inactivity.
Physiotherapy and Rehabilitation
Structured rehabilitation — particularly progressive tendon loading programmes — is the cornerstone of overuse injury management. For tendinopathies, eccentric and heavy slow resistance loading has the most robust evidence base. Rehabilitation also addresses the biomechanical factors — muscle weakness, movement pattern deficiencies, technique errors — that contributed to the injury in the first place.
Regenerative Injections
For overuse injuries that are not responding to load management and physiotherapy, regenerative treatments offer a valuable adjunct.
PRP (Platelet-Rich Plasma) therapy is now widely used in the management of tendinopathy and chronic bursitis. By delivering a concentrated payload of growth factors directly to the pathological tissue, PRP aims to stimulate the repair process that the body has failed to complete on its own. Evidence supports its use in lateral epicondylalgia, rotator cuff tendinopathy, and wrist tendinopathies.
Stem cell therapy may be considered in more significant tendon pathology — partial tears, advanced tendinopathy — where a more potent regenerative stimulus is required.
These treatments are not a shortcut. They work best when combined with a comprehensive rehabilitation programme and appropriate load management.
Surgical Intervention
Surgery is reserved for cases where conservative and regenerative measures have been exhausted, or where structural pathology — such as a significant tendon tear or a complete stress fracture — requires direct repair. In the upper limb, procedures such as arthroscopic tendon debridement, rotator cuff repair, or nerve decompression can produce excellent outcomes when performed by an experienced specialist.
Preventing Overuse Injuries: What the Evidence Supports
Prevention is always preferable to treatment. The following principles are well supported by the sports medicine evidence base.
Manage Training Load Carefully
The most significant risk factor for overuse injury is a rapid increase in training volume or intensity. The commonly cited guideline of no more than a 10% increase in weekly load per week is a reasonable rule of thumb, though the appropriate rate depends on the individual athlete’s conditioning and recovery capacity.
Prioritise Recovery
Training is a stimulus; adaptation happens during recovery. Inadequate sleep, poor nutrition, and insufficient rest between sessions impair the tissue remodelling process and increase injury risk. This is particularly relevant for athletes who train across multiple sessions or disciplines.
Address Technique and Equipment
Biomechanical inefficiencies are a major driver of upper limb overuse injuries. In padel and tennis, grip size, string tension, and stroke mechanics all influence elbow loading. A sports-specific technique assessment — and where necessary, correction — can significantly reduce injury risk.
In the upper limb, scapular control and rotator cuff function are critical. Weaknesses or movement pattern deficiencies in these areas are frequently identified in athletes presenting with shoulder or elbow overuse injuries and must be addressed as part of both treatment and prevention.
Strength and Conditioning
A well-structured strength and conditioning programme that targets the rotator cuff, forearm musculature, and wrist stabilisers provides the physical resilience needed to tolerate training demands. This should be sport-specific, periodised, and progressive.
Seek Early Assessment
Athletes often delay seeking medical advice for overuse injuries, hoping the pain will resolve on its own. In many cases, early intervention — before the tissue has developed significant pathology — leads to faster recovery and a lower risk of recurrence. A sports injury doctor in Dubai with expertise in upper limb conditions can assess the injury accurately and intervene at the point where conservative management is most effective.
Padel Tennis and Elbow Injuries: A Specific Note
Padel is one of the fastest-growing sports in the UAE, and with that growth has come a significant increase in padel-related elbow injuries presenting to orthopaedic clinics. The sport’s technical demands — particularly the wall-play shots that require rapid forearm rotation and the overhead smash — create a repetitive loading pattern on the elbow extensors that predisposes players to lateral epicondylalgia.
Risk factors specific to padel players include:
- Playing frequency exceeding four sessions per week without adequate recovery
- Poor technique on the backhand drive or smash
- Inappropriate racket weight or grip size
- Insufficient forearm and wrist strength relative to playing volume
Prevention in padel players should focus on technique coaching, appropriate equipment selection, and a structured forearm strengthening programme. When symptoms develop, early assessment and load modification are the most effective interventions.
Frequently Asked Questions
How long do overuse injuries take to heal?
This varies significantly depending on the structure involved and how long the injury has been present. Acute tendinopathies with appropriate management may resolve in six to twelve weeks. Chronic conditions that have been present for months may take considerably longer and often require a structured rehabilitation programme.
Should I stop training completely?
Not necessarily. Complete rest is rarely the optimal approach. Load modification — reducing volume and intensity to a tolerable level — combined with targeted rehabilitation is usually more effective than prolonged inactivity.
When should I see a sports injury doctor?
If pain persists beyond two weeks, is limiting your training or performance, or is worsening despite rest, a professional assessment is warranted. Early diagnosis allows for more effective — and faster — management.
Can I train through an overuse injury?
This depends on the severity of the injury and the specific tissue involved. A sports injury specialist can advise on what level of activity is safe and appropriate during the recovery period.
Is surgery always required for overuse injuries?
No. The majority of overuse injuries resolve with appropriate conservative management, including physiotherapy, load modification, and — where indicated — regenerative injections. Surgery is reserved for cases where conservative measures have failed or where significant structural pathology requires direct repair.
Conclusion
Overuse injuries are not inevitable — but they are common, and they demand respect. Understanding the mechanisms behind repetitive strain injury, recognising the early warning signs, and seeking prompt assessment from an experienced sports injury doctor in Dubai are the most important steps any athlete can take to protect their performance and their long-term joint health.
At Dr. Marouane’s clinic in Dubai, athletes across all levels and disciplines receive specialist assessment and evidence-based management for upper limb overuse injuries — from lateral epicondylalgia and rotator cuff tendinopathy to wrist injuries and stress fractures. Contact us on +971 544 226 123 to arrange a consultation.