Stem Cell Treatment for Shoulder Bursitis Healing
Shoulder bursitis is one of the most common causes of persistent shoulder pain — and one of the most frequently mismanaged. Patients often spend months cycling through anti-inflammatory medication and physiotherapy, experiencing temporary relief that never quite resolves the underlying problem. When the pain keeps returning, the assumption is often that surgery is the only remaining option.
In many cases, that assumption is incorrect. Advances in regenerative medicine — particularly stem cell therapy — have opened a new pathway for patients with chronic shoulder bursitis who have not responded adequately to conventional treatment. This is not an experimental fringe; it is an increasingly evidence-supported approach that an experienced shoulder specialist will now consider as part of a structured, non-surgical management plan.
Understanding Shoulder Bursitis
To understand how stem cell therapy helps, it is useful to first understand what is happening in the joint.
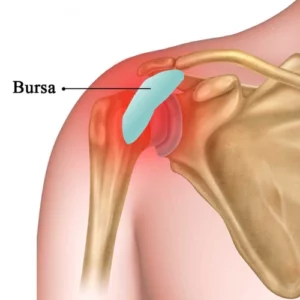
The shoulder contains several bursae — small fluid-filled sacs positioned between tendons, muscles, and bone to reduce friction and allow smooth movement. The largest and most clinically significant is the subacromial bursa, which sits between the rotator cuff tendons and the acromion (the bony prominence at the top of the shoulder).
When this bursa becomes inflamed — through repetitive overhead activity, trauma, impingement, or postural loading — it swells, thickens, and produces excess fluid. The result is pain, particularly with overhead movement and at night, and a restricted, uncomfortable shoulder.
Bursitis rarely exists in complete isolation. It is frequently associated with:
- Shoulder impingement syndrome — where the rotator cuff tendons are compressed as the arm is raised
- Rotator cuff tendinopathy — degenerative changes to the tendons themselves
- Partial rotator cuff tears — which can perpetuate bursitis through altered shoulder mechanics
This is why a surface-level treatment approach — one that addresses only the inflammation without examining the broader picture — so often delivers incomplete results.
Common Symptoms of Shoulder Bursitis
Shoulder bursitis typically presents with a recognisable cluster of symptoms:
- Pain on the outer aspect of the upper arm, often radiating towards the deltoid
- Sharp discomfort when raising the arm above shoulder height
- Pain that worsens at night, particularly when lying on the affected side
- Stiffness and a reduced arc of comfortable movement
- A dull, persistent ache that is present even at rest in more chronic cases
- Tenderness to direct pressure over the shoulder
A key clinical feature is the painful arc — pain that occurs specifically between 60 and 120 degrees of arm elevation, which is characteristic of subacromial impingement and associated bursitis.
Symptoms that have been present for more than three months, or that have failed to respond to two or more courses of conventional treatment, define the condition as chronic — and this is the patient group most likely to benefit from a regenerative approach.
Why Conventional Shoulder Bursitis Treatment Often Fails
The standard approach to shoulder bursitis involves a stepwise progression through several conservative measures.
Rest and Activity Modification
Reducing the activities that aggravate the bursa allows acute inflammation to settle. This is appropriate in the short term but does not address the underlying structural or mechanical cause.
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
NSAIDs reduce inflammation and pain effectively in acute episodes. In chronic bursitis, however, the inflammatory process is more complex and less responsive to systemic medication alone.
Physiotherapy
Targeted physiotherapy — focusing on rotator cuff strengthening, scapular stabilisation, and postural correction — addresses the mechanical contributors to impingement and bursitis. It is an essential component of any management plan and should not be bypassed.
Corticosteroid Injections
Subacromial corticosteroid injections can provide significant, rapid relief and are often an appropriate first-line injectable treatment. However, their benefit is frequently temporary, and repeated injections are associated with potential tendon weakening — a significant concern given the proximity of the rotator cuff.
When symptoms persist despite these measures, the clinical question becomes: what next, before surgery?
Stem Cell Therapy for Shoulder Bursitis: The Regenerative Approach
Stem cell therapy represents a biologically active treatment that goes beyond symptom suppression. Rather than dampening the inflammatory response temporarily, the goal is to provide the tissue with the biological tools it needs to repair and remodel.
How Stem Cells Work in This Context
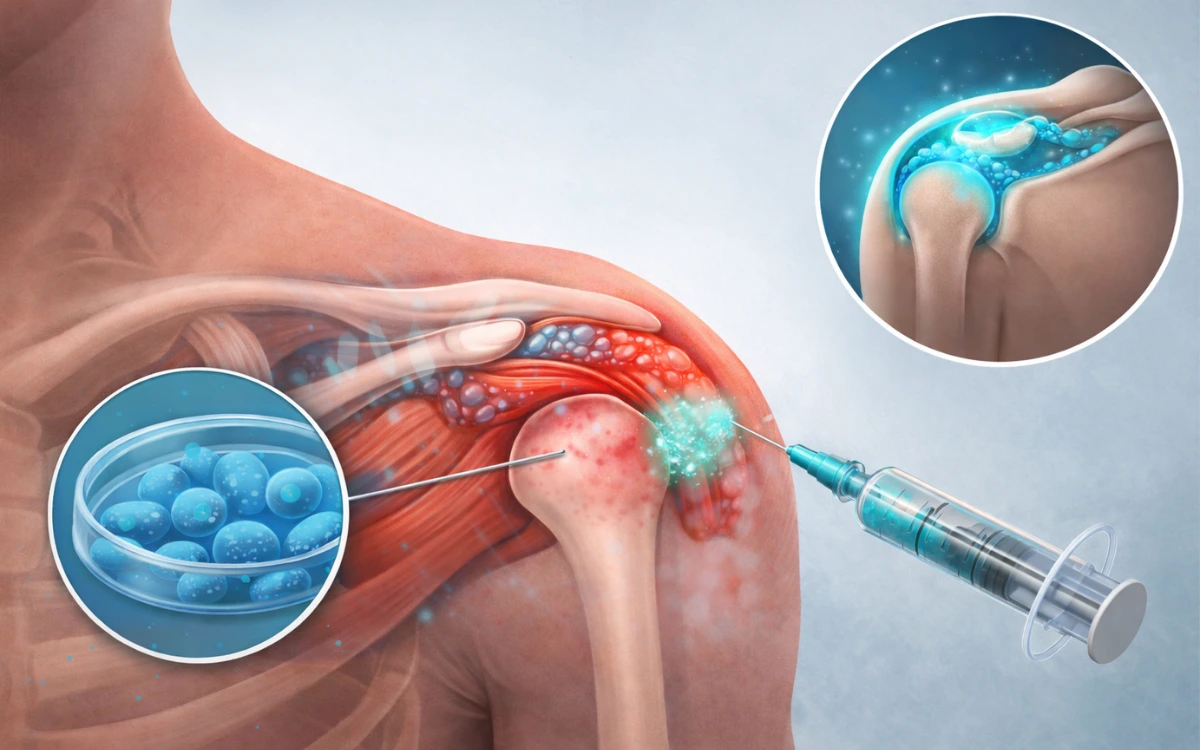
Stem cells — typically harvested from the patient’s own bone marrow or adipose (fat) tissue — are mesenchymal stem cells (MSCs) with the capacity to differentiate into multiple tissue types, including tendon, cartilage, and connective tissue.
When introduced into the subacromial space and surrounding tissue, MSCs exert their effect through two primary mechanisms:
- Paracrine signalling — the cells release a range of bioactive molecules (cytokines, growth factors, and exosomes) that modulate the inflammatory environment, reduce chronic inflammation, and promote tissue healing
- Direct cellular contribution — in appropriate conditions, MSCs can differentiate into local tissue cell types, contributing directly to the repair of damaged tendon and bursal tissue
The result, in clinical practice, is a reduction in chronic inflammation, improvement in tissue quality, and — in many cases — a meaningful reduction in pain and restoration of shoulder function.
What Makes Stem Cell Therapy Different from a Steroid Injection
The distinction is important. A corticosteroid injection suppresses inflammation by interfering with the immune response — it does not repair anything. Stem cell therapy, by contrast, aims to resolve the underlying biological dysfunction. It is a slower, more gradual process, but the effects tend to be more durable.
PRP vs. Stem Cell Therapy: Which Is Right for Shoulder Bursitis?
In the context of shoulder bursitis and impingement, both PRP and stem cell therapy have a role — and the choice between them depends on the severity and chronicity of the condition.
PRP therapy is often the first regenerative option considered. It is a simpler procedure, derived entirely from a blood draw, and is well-suited to mild to moderate bursitis where the primary goal is inflammation reduction and tissue support.
Stem cell therapy is generally considered when:
- Bursitis is chronic and has failed to respond to PRP or other conservative measures
- There is associated tendon pathology (tendinopathy or partial tear) that may benefit from the broader regenerative capacity of stem cells
- The patient is seeking a more comprehensive regenerative intervention
A specialist assessment — including ultrasound or MRI imaging — is necessary to determine which approach is most clinically appropriate for each individual patient.
Who Is a Candidate for Stem Cell Treatment for Shoulder Bursitis?
Stem cell therapy for shoulder bursitis is most appropriate when:
- Symptoms have been present for more than three months (chronic bursitis)
- At least two courses of conventional treatment have not produced lasting relief
- Imaging confirms subacromial bursitis, with or without associated rotator cuff tendinopathy
- The patient is not yet at a stage requiring surgical decompression
- The patient is in good general health and committed to post-treatment rehabilitation
It is not appropriate as a substitute for surgery in cases where structural damage — such as a full-thickness rotator cuff tear — requires direct surgical repair.
The Procedure: What to Expect
Stem cell therapy for shoulder bursitis is performed in an outpatient clinical setting. The procedure does not require general anaesthesia and is typically completed within a single appointment.
The steps involved are:
- Clinical and imaging review — a thorough assessment to confirm diagnosis and identify associated pathology
- Stem cell harvest — a small volume of bone marrow (from the posterior iliac crest) or adipose tissue is collected under local anaesthesia
- Processing — the harvested material is concentrated to isolate the stem cell fraction
- Guided injection — stem cells are injected into the subacromial space and, where indicated, into adjacent tendon tissue under ultrasound guidance
- Observation and discharge — most patients are discharged within a short period and can return home the same day
Some soreness at the harvest site and injection site is expected for two to five days following the procedure.
Recovery and Rehabilitation
Recovery after stem cell treatment is structured but not onerous compared to surgical alternatives.
Key post-treatment guidance includes:
- Avoid anti-inflammatory medications for at least two to four weeks post-injection, as these may impair the regenerative process
- Rest the shoulder from aggravating activities for the first one to two weeks
- Begin guided physiotherapy — typically at two weeks — to restore movement and strengthen the supporting musculature
- Attend follow-up appointments at six and twelve weeks to assess progress
Improvement is gradual. Most patients notice meaningful change at six to eight weeks, with continued progress over three to six months. In some cases, a second injection may be considered if the initial response is partial.
Setting Realistic Expectations
Stem cell therapy is not a guaranteed cure for shoulder bursitis, and it does not work equally well for every patient. Results depend on the chronicity and severity of the condition, the presence of associated pathology, age, general health, and the quality of post-treatment rehabilitation.
What the evidence consistently supports is that in appropriately selected patients, stem cell therapy can deliver:
- Sustained reduction in chronic shoulder pain
- Improved range of motion and shoulder function
- Delayed or avoided surgical intervention
- Better tissue quality on follow-up imaging
These outcomes are clinically meaningful — and for many patients, they represent a significant improvement in quality of life.
Frequently Asked Questions
Is stem cell therapy for shoulder bursitis safe? Yes. When performed by a qualified specialist using the patient’s own cells, the risk of adverse reaction is very low. The procedure has a well-established safety profile in musculoskeletal medicine.
How long do the results last? Results vary, but many patients report sustained improvement for one to two years or longer. The durability of response depends on the severity of the underlying condition and adherence to post-treatment rehabilitation.
How is this different from a cortisone injection? A cortisone injection suppresses inflammation temporarily. Stem cell therapy aims to resolve the underlying tissue dysfunction — it is a biological repair process, not a suppression of symptoms.
Will I need time off work? Most patients with desk-based roles can return to work within a few days. Those in physically demanding roles may require a short period of modified duties.
Is it painful? Local anaesthesia is used throughout the procedure. Some soreness afterwards is normal and typically manageable with simple analgesia.
Conclusion
Chronic shoulder bursitis that has not responded to conventional treatment is not a condition that patients simply have to live with — nor does it inevitably require surgery. Stem cell therapy, applied by an experienced shoulder specialist, offers a biologically grounded, minimally invasive route to lasting relief.
At Dr. Marouane’s clinic in Dubai, patients with persistent shoulder pain receive a thorough diagnostic assessment and a personalised treatment plan tailored to the severity and nature of their condition. If you have been struggling with chronic shoulder bursitis, contact us on +971 544 226 123 to discuss whether regenerative medicine is the right next step for you.