Osteoarthritis in Joints: Types, Causes, Diagnosis & Treatment Options
Osteoarthritis is the most common joint condition in the world, and yet it remains widely misunderstood — both by patients who assume it is simply an inevitable consequence of ageing, and by those who believe that surgery is the only meaningful treatment. Neither assumption is accurate.
Osteoarthritis is a progressive, degenerative disease of the joint, characterised by the breakdown of articular cartilage, changes to the underlying bone, and — in most cases — a degree of inflammation that contributes significantly to the pain and stiffness patients experience. Understanding the condition properly is the first step towards managing it effectively. And effective management, in most cases, does not begin with surgery — it begins with accurate diagnosis, appropriate conservative care, and increasingly, with regenerative treatments that can meaningfully alter the course of the disease.
What Is Osteoarthritis?
Articular cartilage is a remarkable tissue. It covers the ends of bones within synovial joints, providing a smooth, low-friction surface that allows movement with minimal wear. It also acts as a shock absorber, distributing compressive loads across the joint surface. In a healthy joint, it does this silently and efficiently for decades.
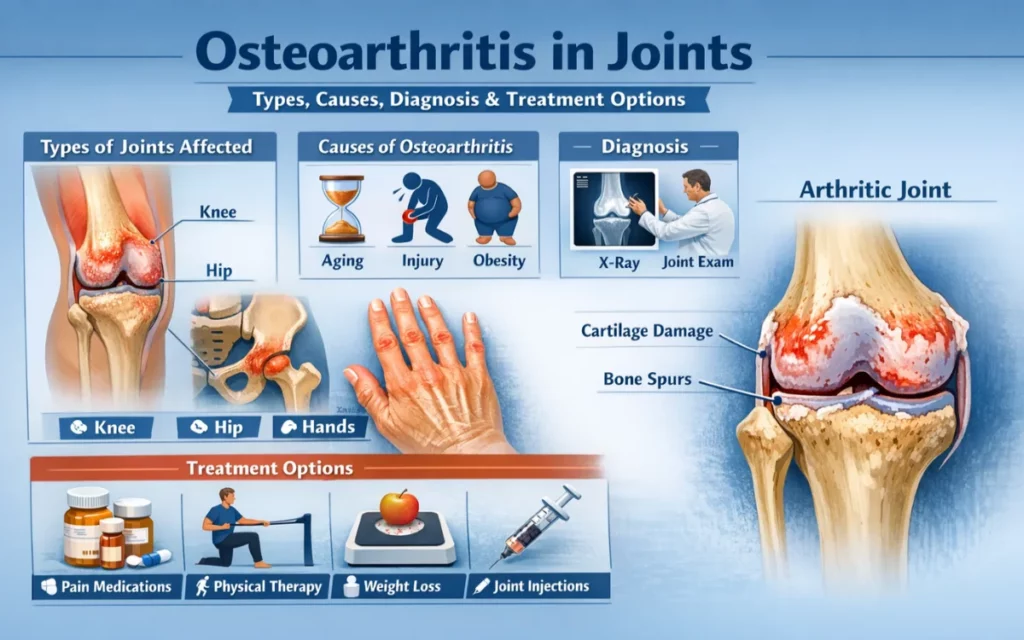
In osteoarthritis, this cartilage gradually breaks down. As it thins and becomes irregular, the underlying bone is exposed to greater stress. The bone responds by remodelling — thickening in some areas, forming osteophytes (bone spurs) at the joint margins, and in some cases developing subchondral cysts. The synovium (joint lining) becomes inflamed, producing excess fluid and contributing to swelling and pain.
This process is not purely mechanical. Biochemical changes within the cartilage — particularly an imbalance between cartilage-building and cartilage-degrading enzymes — drive the degenerative cycle, which is why osteoarthritis is now understood as a disease of the whole joint, not simply a case of “worn-out cartilage.”
Which Joints Are Most Commonly Affected?
Osteoarthritis can affect any synovial joint, but it tends to develop in those subjected to the greatest cumulative load. In Dr. Marouane’s specialist practice, the joints most frequently presenting with osteoarthritis are:
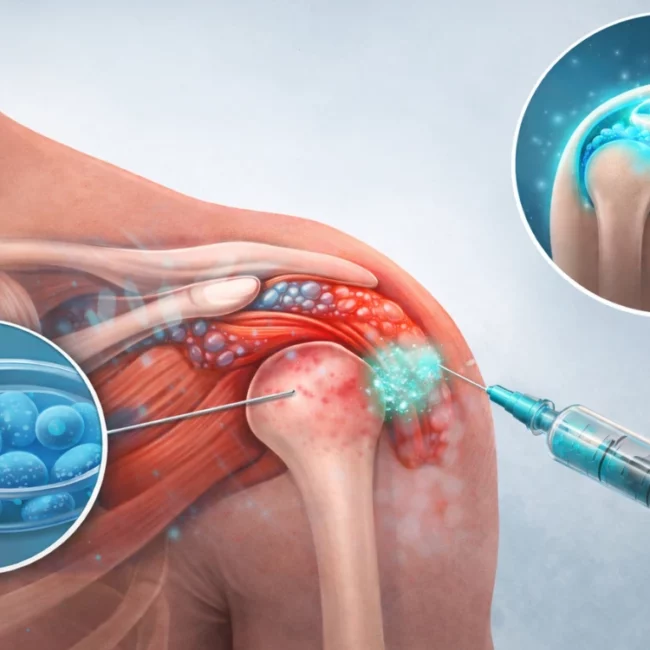
The shoulder — often developing after years of overhead activity, prior injury, or rotator cuff pathology. Glenohumeral osteoarthritis can cause deep, aching shoulder pain, progressive loss of rotation, and — in advanced cases — significant restriction of daily function.
The elbow — less common than shoulder or wrist osteoarthritis, but frequently seen in patients with a history of heavy manual work, repetitive throwing, or prior elbow fracture. Elbow osteoarthritis is characterised by loss of terminal extension and flexion, pain at the end of range, and — in some cases — locking caused by intra-articular loose bodies.
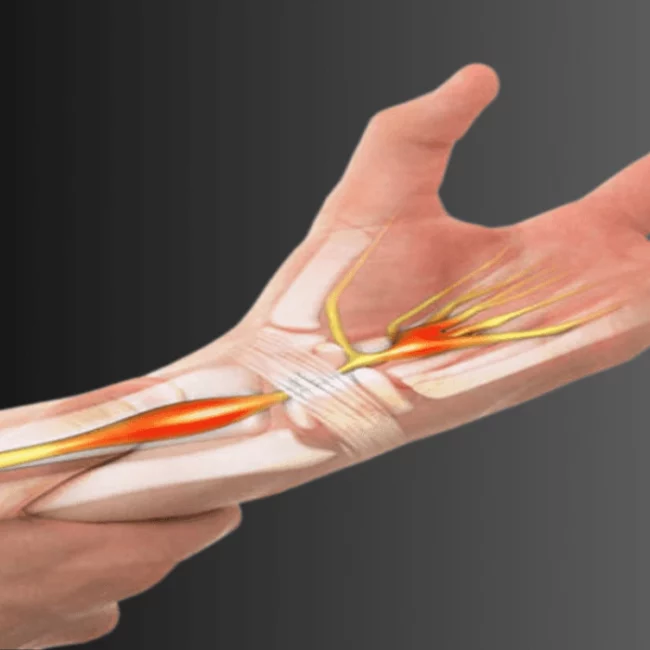
The wrist — frequently post-traumatic, developing after scaphoid fractures, distal radius fractures, or ligament injuries that alter the load distribution across the carpal bones. Wrist osteoarthritis can develop in younger patients and is a common source of persistent wrist pain in those with a history of hand or wrist injury.
The finger and thumb joints — particularly the carpometacarpal (CMC) joint of the thumb, which is one of the most common sites of osteoarthritis in women over 50. Thumb base arthritis causes pain at the base of the thumb, weakness of pinch grip, and a characteristic aching with activities such as opening jars or turning keys.
Causes and Risk Factors
Osteoarthritis is multifactorial. No single cause explains every case, but the following risk factors are well established:
Age — the most consistent risk factor. The prevalence of osteoarthritis increases significantly after the age of 50, reflecting cumulative cartilage stress over time.
Prior joint injury — post-traumatic osteoarthritis accounts for a significant proportion of cases in younger patients. Fractures that involve the joint surface, ligament injuries that alter joint mechanics, and episodes of dislocation all increase long-term arthritis risk.
Occupation and repetitive loading — sustained physical demands placed on specific joints over years can accelerate cartilage breakdown. Manual labourers, professional athletes, and those in repetitive occupational roles are at higher risk.
Anatomical factors — joint shape, alignment, and the distribution of mechanical load across the joint surface all influence susceptibility to osteoarthritis. Some individuals have anatomical configurations that place them at inherently higher risk.
Genetics — there is a clear heritable component to osteoarthritis, particularly in hand and thumb arthritis.
Sex — women develop osteoarthritis more frequently than men, particularly in the hand, thumb, and knee. Hormonal factors are thought to play a role, though the precise mechanisms are not fully understood.
Diagnosing Osteoarthritis: What a Specialist Assessment Involves
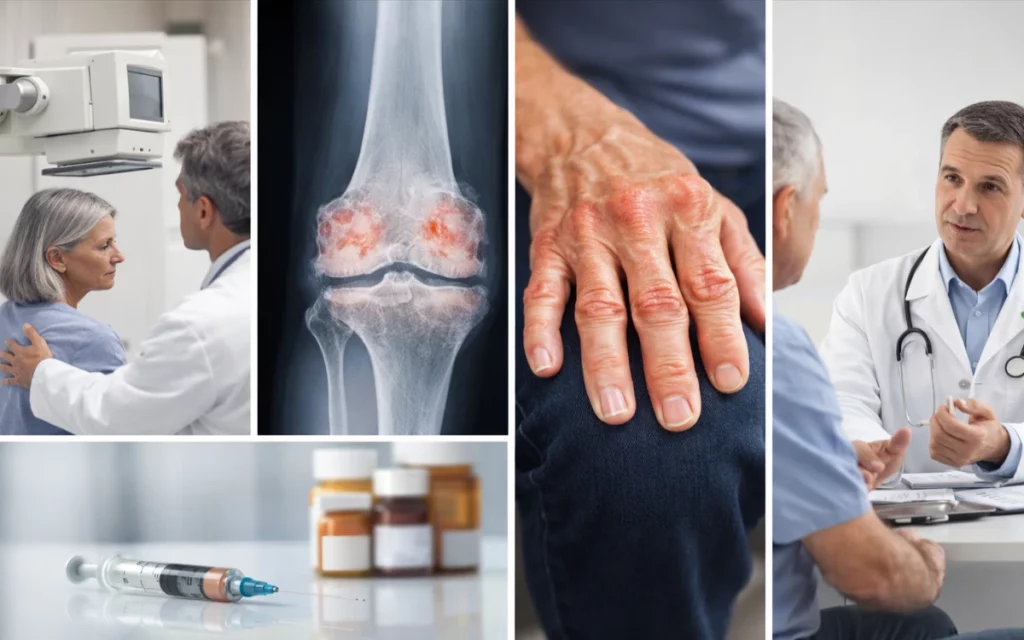
Diagnosis of osteoarthritis is primarily clinical, supported by imaging. A thorough assessment by an experienced orthopaedic specialist will include:
Clinical History
A detailed history is essential — not simply to confirm the diagnosis, but to understand the pattern of symptoms, the rate of progression, the functional impact, and the patient’s goals and expectations. Key questions include: Which activities provoke pain? How has function changed over time? Has the joint ever been injured? What treatments have been tried?
Physical Examination
Examination of the affected joint assesses range of motion (active and passive), the presence of swelling or effusion, crepitus on movement, joint line tenderness, and the stability of surrounding ligaments and soft tissues. In the hand and wrist, grip and pinch strength are measured objectively.
Imaging
Plain X-rays remain the first-line imaging investigation for osteoarthritis. Classic findings include joint space narrowing (reflecting cartilage loss), subchondral sclerosis, osteophyte formation, and — in advanced cases — subchondral cysts. It is important to note that X-ray findings do not always correlate directly with symptom severity; some patients with significant radiographic changes have relatively mild symptoms, and vice versa.
Ultrasound is useful for assessing synovial inflammation, joint effusion, and periarticular soft tissue pathology.
MRI provides detailed characterisation of cartilage, bone, and soft tissue changes and is particularly useful when the diagnosis is uncertain, when associated pathology (such as a ligament injury or tendon tear) is suspected, or when planning surgical intervention.
Osteoarthritis Treatment: A Structured Approach
The management of osteoarthritis is best understood as a staged, individualised process. Treatment decisions are guided by the severity of symptoms, the degree of joint damage on imaging, the patient’s age and activity level, and their personal priorities.
Stage 1: Education and Lifestyle Modification
Patient education is a genuinely effective intervention. Understanding the nature of osteoarthritis — that it is manageable, that pain does not always mean damage, and that activity is generally beneficial — changes how patients engage with their condition and improves outcomes.
Lifestyle modifications that support joint health include:
- Weight management (for joints bearing body weight)
- Regular low-impact exercise to maintain joint mobility and periarticular muscle strength
- Activity modification to reduce peak joint loading without eliminating activity
Stage 2: Physiotherapy and Exercise
A structured physiotherapy programme is one of the most effective interventions for osteoarthritis at any stage. The goals are to maintain or improve range of motion, strengthen the muscles that support and unload the joint, and optimise movement patterns to reduce unnecessary joint stress.
For upper limb osteoarthritis, physiotherapy programmes focus on rotator cuff and scapular strengthening (shoulder), forearm and wrist strengthening (elbow and wrist), and hand therapy with specific grip and pinch training (hand and thumb arthritis).
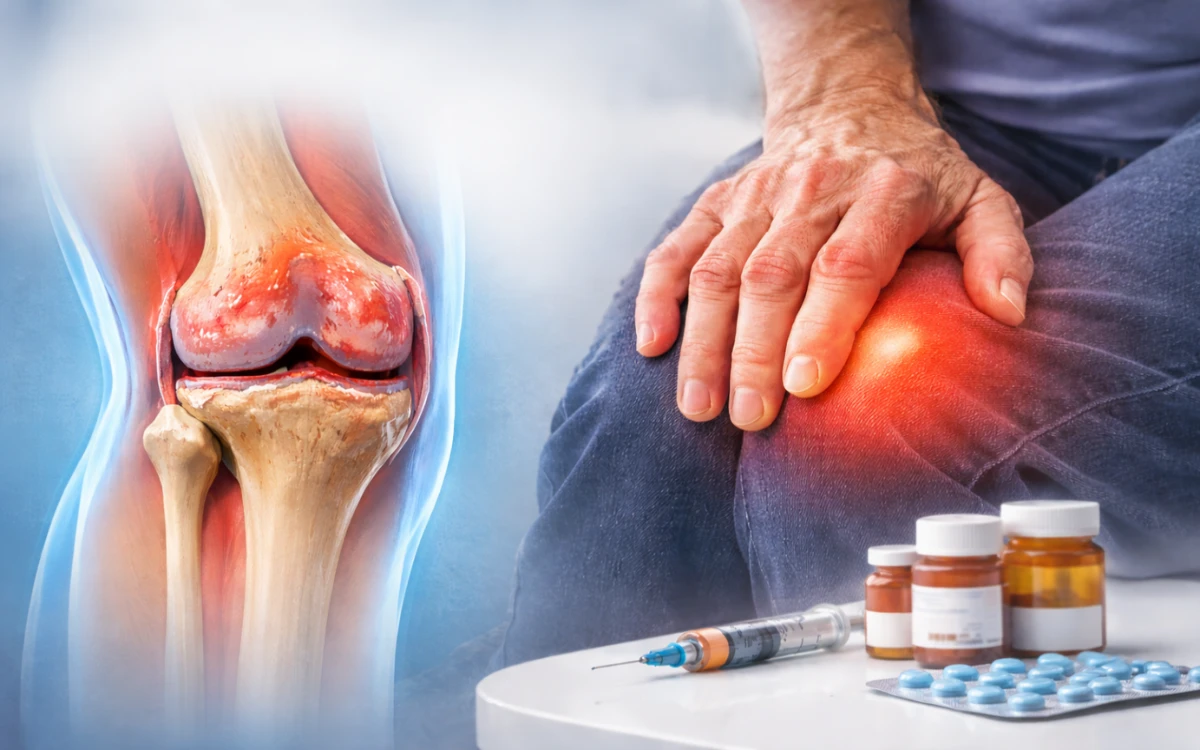
Stage 3: Analgesia and Anti-Inflammatory Treatment
Pharmacological management plays a supporting role. Topical and oral NSAIDs reduce inflammation and pain in the short to medium term. They are most useful during flare-ups and as an adjunct to active rehabilitation, rather than as a standalone long-term strategy.
Stage 4: Injectable Treatments
When physiotherapy and analgesia provide insufficient relief, injectable treatments are the next step.
Corticosteroid injections offer reliable short-term pain relief and are appropriate for acute flares and for patients in whom rapid symptom control is needed. Their long-term use is limited by the potential for accelerated cartilage degradation with repeated administration.
Viscosupplementation (hyaluronic acid injections) delivers a synthetic joint lubricant directly into the joint. Evidence is variable across studies, but some patients — particularly in early to moderate osteoarthritis — report meaningful and sustained benefit.
PRP (Platelet-Rich Plasma) therapy is increasingly well-supported by evidence as an injectable treatment for osteoarthritis. By concentrating the patient’s own growth factors and delivering them intra-articularly, PRP aims to reduce chronic inflammation, support the maintenance of remaining cartilage, and improve joint function. In upper limb osteoarthritis, PRP offers a regenerative option that goes beyond symptom suppression.
Stem cell therapy represents the most biologically comprehensive injectable option currently available. Mesenchymal stem cells derived from bone marrow or adipose tissue can modulate inflammation, release regenerative signalling molecules, and — in appropriate conditions — contribute to cartilage repair. Stem cell therapy is most likely to benefit patients with moderate osteoarthritis and significant cartilage involvement who have not responded adequately to other injectable treatments.
Stage 5: Surgical Intervention
Surgery is considered when non-operative management has been exhausted and joint damage is severe enough to justify the risks and recovery demands of an operative procedure.
In the upper limb, surgical options include:
- Arthroscopic debridement — removal of loose bodies, osteophytes, and inflamed synovium. Most beneficial in early to moderate disease with specific intra-articular pathology.
- Joint replacement — total or partial replacement of the affected joint surfaces with prosthetic components. Relevant in end-stage glenohumeral osteoarthritis, elbow arthritis, and wrist arthritis.
- Joint fusion (arthrodesis) — in selected cases, particularly wrist arthritis, fusion eliminates pain at the cost of movement. Appropriate in patients for whom pain relief is the primary goal.
The decision to proceed with surgery is never taken lightly and always follows a detailed discussion of the patient’s goals, expectations, and the likely outcomes and limitations of the procedure.
The Role of Regenerative Medicine in Osteoarthritis Treatment
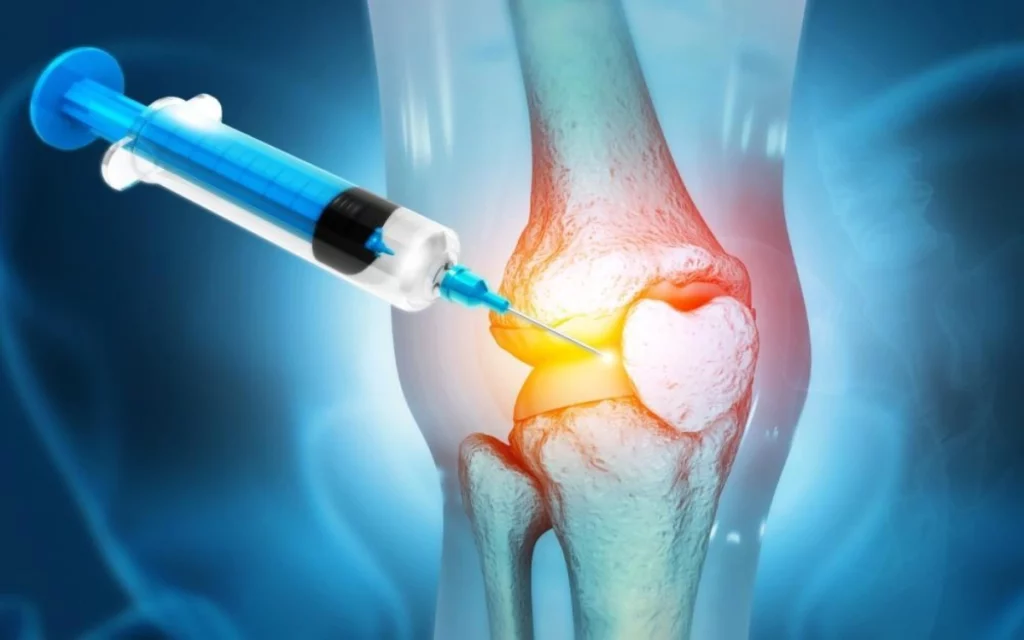
As outlined above, both PRP and stem cell therapy have an established and growing role in the non-surgical management of osteoarthritis. They are most effective when:
- Arthritis is mild to moderate (Kellgren-Lawrence grade 1–3 on X-ray)
- Significant cartilage remains within the joint
- The patient has not responded adequately to conservative management alone
- Surgery is not yet indicated — or the patient wishes to exhaust non-operative options first
Regenerative medicine does not reverse established structural damage. What it offers is a biologically active treatment that targets the mechanisms driving joint deterioration, provides sustained symptom relief, and may slow disease progression — outcomes that no currently available pharmaceutical can match.
Frequently Asked Questions
Is osteoarthritis inevitable as I get older? Age is a risk factor, not a guarantee. Many people in their 70s and 80s have minimal arthritis, while others develop significant disease in their 40s or 50s. Lifestyle, occupation, prior injury, and genetics all play a role.
Does exercise make osteoarthritis worse? No — in fact, the evidence consistently shows that appropriate exercise is one of the most effective treatments for osteoarthritis. The key is exercise that is suited to the stage of the condition and the affected joint. A physiotherapist or orthopaedic specialist can advise on the right programme.
How do I know if I need surgery? Surgery is appropriate when symptoms are severe, significantly limiting daily function, and not responding to non-operative treatment — and when imaging confirms structural damage that warrants operative intervention. This decision should always be made after a thorough assessment and discussion with an experienced orthopaedic specialist.
Can osteoarthritis be cured? There is currently no treatment that can completely reverse established osteoarthritis. However, it can be managed very effectively — with many patients achieving significant pain reduction, maintained function, and a good quality of life through appropriate treatment.
What is the best first step if I think I have osteoarthritis? Seek assessment from a qualified orthopaedic specialist. An accurate diagnosis — including imaging — is the foundation of effective management. Early intervention generally leads to better outcomes.
Conclusion
Osteoarthritis is a complex, progressive condition — but it is not one that patients have to simply accept. With accurate diagnosis, a structured and individualised treatment approach, and access to modern regenerative therapies, the majority of patients can achieve meaningful improvement in pain and function without rushing to surgery.
At Dr. Marouane’s clinic in Dubai, patients with osteoarthritis of the shoulder, elbow, wrist, or hand receive specialist assessment and a personalised management plan that reflects the severity of their condition and their individual goals. If you are experiencing persistent joint pain and would like expert advice on your options, contact us on +971 544 226 123 to arrange a consultation.