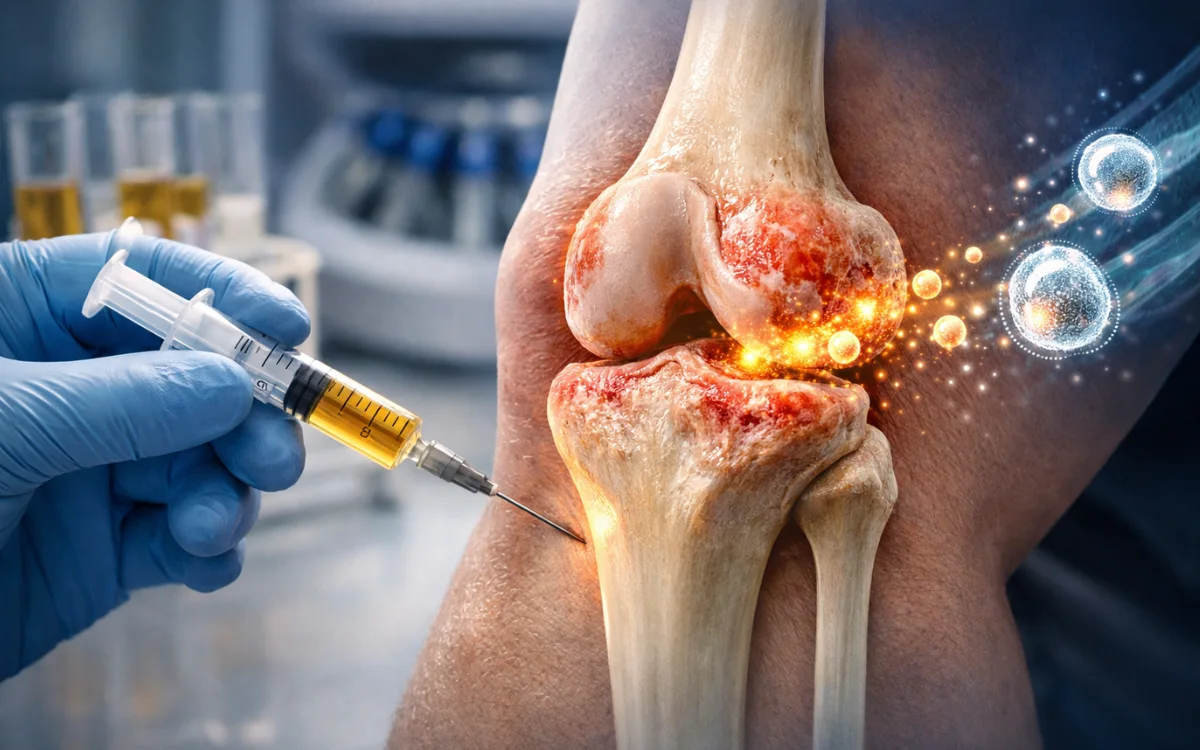
Regenerative Medicine for Knee Arthritis Treatment
Knee arthritis is one of the most prevalent musculoskeletal conditions seen in orthopaedic practice and one of the most undertreated. Many patients spend years managing pain with medication and periodic steroid injections, gradually accepting a reduction in their activity and quality of life as an inevitable consequence of the condition. By the time they seek specialist advice, they often arrive with one question: Is knee replacement the only option left?
In the majority of cases, the answer is no. Regenerative medicine has fundamentally changed the non-surgical management of knee arthritis, offering treatments that go beyond symptom suppression to target the biological processes driving joint deterioration. For patients in the early to moderate stages of knee arthritis and even some in more advanced disease, this represents a genuinely meaningful shift in what is achievable without surgery.
What Is Knee Arthritis?
The knee is the largest synovial joint in the body, bearing the combined demands of
weight-bearing and dynamic movement across decades of daily use. The articular surfaces, the ends of the femur, tibia, and the underside of the patella are lined with hyaline cartilage, a dense, resilient tissue that allows near-frictionless movement and distributes compressive loads across the joint.
Knee arthritis occurs when this cartilage breaks down. As it thins and becomes irregular, the underlying subchondral bone is exposed to increased stress. The bone responds by remodelling, forming osteophytes (bone spurs) at the joint margins, thickening, and in some cases developing cystic changes. The synovium becomes chronically inflamed, producing excess fluid and biochemical mediators that perpetuate the degenerative cycle.
The result is a joint that is painful, stiff, and progressively less functional.
Types of Knee Arthritis
Osteoarthritis is by far the most common form. It is primarily degenerative, driven by cumulative mechanical wear combined with biochemical changes within the cartilage matrix. It tends to develop gradually over the years and is most prevalent in patients over 50, though it is increasingly seen in younger patients with a history of knee injury or surgery.
Rheumatoid arthritis is an autoimmune condition in which the immune system attacks the synovial lining of the joint, causing persistent inflammation, cartilage damage, and in progressive disease, structural joint destruction. It is a systemic condition that often affects multiple joints simultaneously and requires specialist rheumatological input alongside orthopaedic management.
Post-traumatic arthritis develops as a consequence of prior knee injury, such as anterior cruciate ligament (ACL) tears, meniscal injuries, intra-articular fractures, or episodes of dislocation. Even injuries that were treated appropriately and appeared to heal well can alter joint mechanics sufficiently to accelerate cartilage breakdown over the following years or decades.
Recognising the Symptoms of Knee Arthritis
Knee arthritis rarely presents dramatically. It tends to develop insidiously, with symptoms that worsen gradually over months or years.
Common presentations include:
- Pain — initially provoked by activity, particularly loading activities such as walking, stair climbing, and rising from a chair; later occurring at rest and overnight
- Morning stiffness — typically lasting less than 30 minutes in osteoarthritis (prolonged stiffness suggests an inflammatory arthropathy)
- Swelling — caused by synovial inflammation and excess joint fluid
- Crepitus — a grinding or crunching sensation during knee movement
- Reduced range of motion — difficulty fully straightening or bending the knee
- Joint line tenderness — localised to the medial or lateral compartment, depending on the distribution of disease
- Functional limitation — progressive difficulty with previously straightforward activities
It is clinically important to distinguish which compartment of the knee is predominantly affected medial, lateral, or patellofemoral as this influences both the treatment approach and the choice of surgical intervention if that stage is reached.
Why Conventional Knee Arthritis Treatment Often Falls Short
The standard stepwise management of knee arthritis analgesia, physiotherapy, injections, and eventually surgery is appropriate in principle but frequently inadequate in practice.
Understanding where each modality falls short helps clarify the role that regenerative medicine plays.
Analgesia and NSAIDs
Paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) reduce pain and inflammation and are a reasonable first-line intervention. However, they have no disease-modifying effect they manage symptoms without altering the underlying joint pathology. Long-term NSAID use also carries meaningful gastrointestinal, renal, and cardiovascular risks.
Physiotherapy
Structured physiotherapy is one of the most effective interventions for knee arthritis and should be a component of every management plan. Quadriceps strengthening, in particular, reduces the load experienced by the joint and is strongly supported by evidence. The limitation of physiotherapy alone is that it cannot reverse cartilage damage, and its benefit may plateau in moderate to advanced disease.
Corticosteroid Injections
Intra-articular corticosteroid injections offer reliable, often rapid pain relief in the short term, typically lasting weeks to a few months. They are most useful for managing acute inflammatory flares. However, evidence suggests that repeated corticosteroid injections may accelerate cartilage degradation over time, and their role in long-term management is therefore limited.
Viscosupplementation
Hyaluronic acid injections supplement the natural lubricating properties of synovial fluid. Evidence for efficacy is variable, but some patients particularly those with early to moderate osteoarthritis report sustained benefit.
The gap in this management ladder between failing conservative measures and the major step of joint replacement is precisely where regenerative medicine has the most to offer.
Regenerative Medicine for Knee Arthritis: The Clinical Case
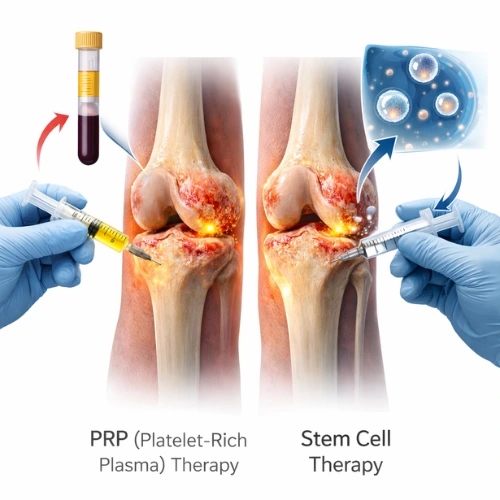 Regenerative medicine refers to biologically active treatments that harness the body’s own repair mechanisms to target joint pathology at the tissue level. In the context of knee arthritis, this means reducing chronic intra-articular inflammation, supporting the maintenance and repair of remaining cartilage, and improving the biological environment within the joint.
Regenerative medicine refers to biologically active treatments that harness the body’s own repair mechanisms to target joint pathology at the tissue level. In the context of knee arthritis, this means reducing chronic intra-articular inflammation, supporting the maintenance and repair of remaining cartilage, and improving the biological environment within the joint.
The two most established and clinically applied options are PRP therapy and stem cell therapy.
PRP (Platelet-Rich Plasma) Therapy
PRP is prepared from the patient’s own blood. A small venous sample is drawn, centrifuged to concentrate the platelet fraction, and injected directly into the knee joint under ultrasound guidance.
Platelets are not simply clotting agents they carry a rich payload of growth factors, including PDGF (platelet-derived growth factor), TGF-β (transforming growth factor beta), and IGF-1
(insulin-like growth factor), and VEGF (vascular endothelial growth factor). These molecules play active roles in tissue repair, inflammation modulation, and the regulation of cartilage metabolism.
When delivered into an arthritic knee joint, PRP creates a pro-healing environment that can:
- Reduce chronic synovial inflammation
- Slow the rate of cartilage degradation
- Stimulate the activity of chondrocytes (cartilage cells)
- Improve pain, stiffness, and functional range of motion
Because PRP is derived entirely from the patient’s own biology, the risk of adverse reaction is exceptionally low. Most patients notice progressive improvement over four to eight weeks, with effects that often persist for six to twelve months or longer. For patients with mild to moderate knee arthritis, PRP represents a well-evidenced, minimally invasive option that sits meaningfully ahead of corticosteroid injections in terms of both duration and biological effect.
Stem Cell Therapy
Stem cell therapy represents the most biologically comprehensive regenerative option currently available for knee arthritis. Mesenchymal stem cells (MSCs), typically harvested from the patient’s own bone marrow or adipose (fat) tissue, are multipotent cells capable of differentiating into cartilage, bone, and connective tissue cell types.
When introduced into the knee joint, MSCs exert their effect through two primary mechanisms:
Paracrine signalling — MSCs release a range of bioactive molecules, including cytokines, growth factors, and extracellular vesicles (exosomes), that modulate the inflammatory environment, promote tissue repair, and influence the behaviour of local cells.
Direct cellular contribution — in appropriate conditions, MSCs can differentiate into chondrocytes, potentially contributing directly to cartilage repair and regeneration.
The clinical result in appropriately selected patients is a meaningful reduction in chronic inflammation, improvement in cartilage quality, and sustained improvement in pain and function.
Stem cell therapy is generally considered when:
- Arthritis is moderate to moderately advanced
- Cartilage damage is more significant and PRP alone may not provide sufficient regenerative stimulus
- The patient is seeking a more durable regenerative intervention before committing to joint replacement
The procedure is performed in an outpatient setting, does not require general anaesthesia, and is considerably less invasive than any surgical alternative.
Who Is a Suitable Candidate?
Patient selection is fundamental to achieving good outcomes with regenerative knee treatments. A thorough clinical and imaging assessment is essential before any treatment decision is made.
Regenerative medicine for knee arthritis is most appropriate when:
- Arthritis is confirmed on imaging as mild to moderate (Kellgren-Lawrence grade 1–3)
- Significant cartilage remains within the joint regenerative treatments require viable tissue to work with
- Symptoms are persistent and significantly affecting the quality of life despite adequate conservative management
- The patient wishes to delay or avoid knee replacement
- The patient is in reasonable general health and committed to post-treatment rehabilitation
Advanced end-stage arthritis with bone-on-bone contact across the entire joint compartment is less likely to respond to regenerative treatment alone. In these cases, regenerative therapy may still offer symptomatic benefit, but joint replacement may ultimately be the most appropriate long-term solution.
What to Expect: The Procedure
Both PRP and stem cell injections for knee arthritis are performed as outpatient procedures.
PRP procedure:
- Clinical and imaging review
- Venous blood draw (typically 15–30ml)
- Centrifugation to concentrate the platelet fraction
- Ultrasound-guided injection into the knee joint
- Short observation period and same-day discharge
Stem cell procedure:
- Clinical and imaging review
- Bone marrow harvest from the posterior iliac crest, or adipose harvest, performed under local anaesthesia
- Processing and concentration of the MSC fraction
- Allogenic safe stem cells from the umbilical cord to avoid invasive procedures
- Ultrasound-guided injection into the knee joint, with additional periarticular injection where indicated
- Observation and same-day discharge
Some soreness at the harvest site and injection site is expected for two to five days following stem cell treatment. PRP injections typically produce milder post-procedure discomfort.
Recovery and Post-Treatment Rehabilitation
 Recovery following regenerative knee treatment is structured and progressive, but considerably less demanding than post-surgical rehabilitation.
Recovery following regenerative knee treatment is structured and progressive, but considerably less demanding than post-surgical rehabilitation.
Key guidance in the post-treatment period includes:
- Avoid NSAIDs for at least two to four weeks following the injection. Anti-inflammatory medications can interfere with the biological healing response that the treatment is designed to stimulate
- Relative rest from high-impact activities for the first one to two weeks
- Begin physiotherapy at approximately two weeks post-injection, focusing on quadriceps strengthening, range of motion, and functional movement patterns
- Attend follow-up appointments at six and twelve weeks to assess progress and guide ongoing management
Improvement is gradual and progressive. Most patients notice meaningful change at four to eight weeks, with continued gains developing over three to six months. In some cases, particularly following PRP, a repeat injection at six to twelve months may extend or consolidate the benefit.
Setting Realistic Expectations
Regenerative medicine for knee arthritis is not a cure. It cannot reconstruct cartilage that has been completely lost, and it will not restore a severely degenerated joint to its pre-arthritic state. What it can do when applied correctly, to the right patient, at the right stage of disease is deliver sustained, clinically meaningful improvements in pain and function that significantly alter the patient’s quality of life and trajectory.
For many patients, that means continuing to work, exercise, and live actively for years without the recovery demands and lifestyle adjustments that joint replacement surgery requires. That is a genuinely significant outcome, and one that deserves to be taken seriously as part of a well-considered management plan.
Frequently Asked Questions
1. Is regenerative medicine for knee arthritis safe?
Yes, when performed by a qualified orthopaedic specialist. PRP uses the patient’s own blood, eliminating the risk of rejection or allergic reaction. Stem cell procedures carry a slightly higher procedural involvement but have a well-established safety profile in musculoskeletal medicine.
2. How long do the results last?
PRP typically provides relief for six to twelve months; many patients report longer benefit with repeat treatment. Stem cell therapy tends to offer more durable results in appropriate candidates, with many patients reporting sustained improvement for one to two years or longer.
3. How many sessions are needed?
For PRP, some patients benefit from a single injection; others may have a course of two to three injections at intervals. Stem cell therapy is typically assessed as a single procedure before further treatment decisions are made.
4. Can I avoid knee replacement?
In early- to moderate-stage knee arthritis, regenerative medicine may significantly delay surgery or, in some cases, avoid it altogether. In advanced disease, it may still provide meaningful symptomatic benefit but is unlikely to replace the need for joint replacement indefinitely.
5. How soon can I return to normal activity?
Most patients can return to light daily activities within a few days. Return to sport and higher-impact activity is typically guided by the physiotherapy programme, usually from six to twelve weeks post-treatment, depending on the individual response.
6. Is the procedure painful?
Local anaesthesia is used throughout. Most patients experience minimal discomfort during the injection itself. Some soreness in the days following is normal and manageable with simple analgesia (avoiding NSAIDs).
7. Are the stem cells from the umbilical cord safe enough to be used for knee arthritis?
When sourced from certified laboratories and used by experienced physicians, umbilical cord MSC therapy appears safe and promising for knee osteoarthritis, but ongoing research continues to refine its indications and long-term effectiveness
Conclusion
Knee arthritis does not have to follow an inevitable path from pain management to surgery. Regenerative medicine applied at the right stage, by an experienced specialist, and supported by structured rehabilitation offers a biologically grounded, minimally invasive route to sustained pain relief and improved joint function.
At Dr Marouane’s clinic in Dubai, patients with knee arthritis receive a comprehensive assessment and an individualised treatment plan based on the severity of their condition and their personal goals. If you are living with persistent knee pain and want to understand your options before committing to surgery, contact us on +971 544 226 123 to arrange a consultation.


